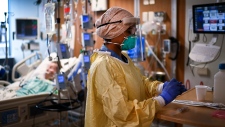
Provincial health officials say they are aiming to increase capacity in the hospital system to somewhere between 110 and 115 per cent by late fall in order to deal with the backlog of surgeries and procedures that built up during Ontario’s COVID-19 lockdown, though they declined to give an estimate for how many people may be part of the backlog.
Officials said Wednesday that they will spend $324 million to try and work through the backlog, adding 67,000 additional surgeries and procedures between October and spring 2022.
The plan includes $35 million for more MRI and CT scans, $18 million for a centralized surgical waitlist management system, $1 million for surgical “smoothing” and coaching and $24 million to increase the volume of surgical and diagnostic services in independent health facilities.
To help work through the backlog, surgeries will also be carried out at night and on weekends.
To support the surgical ramp-up, the province is also offering up to 200 nurses a $10,000 incentive this year in exchange for a one-year practice commitment and is offering “surgical extender” training programs to as many as 500 existing nurses to improve their skills.
The province said its plan is based on wait times for “actual” numbers of patients moving through the system.
Provincial officials said that some wait times actually decreased during the pandemic, but acknowledged that many people who would normally have sought treatment did not do so during lockdown.
The province would not provide a figure for the number of people believed to be part of the backlog.
“What we're looking at our actual volumes of surgeries that need to be done rather than the model numbers,” Health Minister Christine Elliott told reporters during a video news conference Wednesday. “So some of the modeling may have double counted people, may have had them in several different lineups so that those are not the numbers that we're working with. We're looking at the real numbers of actual people on waitlists and that does make a difference in terms of the timing of course how long it would take to deal with those numbers.”
Ontario Health CEO Matt Anderson said that there are around 200,000 people currently on provincially-tracked wait lists, but that number is similar to what would normally be expected. He said that’s because there are many people who have not yet entered the system through diagnosis and referral and said putting a number on the backlog group is “very difficult to do.”
“It's not so much about working in reverse. It's about looking forward,” Anderson said. “This investment is in anticipation that we will see more people coming through.”
Health officials said that while many people did not seek treatment during lockdown, many of those who are part of the backlog belong to the category of high-volume, non-urgent scheduled surgeries and said that group will be the focus in the coming months.
In May, Ontario’s Financial Accountability Office projected that the cancelled surgery backlog would reach 419,200 procedures by the end of September and estimated that it would cost the province $1.3 billion over three and a half years to clear the backlog.
That was based on hospitals operating at 111 per cent of their usual capacity.
Elliott said Wednesday that it is difficult to say how long it will take.
“I think it's difficult to put an exact timeline on it right now because there are some people that are going to become coming forward, they just haven't been diagnosed yet,” she said.
The government said hospitals will find out in early fall how much funding they are getting to perform additional surgeries.
The province said it will “closely monitor” surgical outputs and wait times and will “implement additional measures if needed.”
Former chief medical officer of health Dr. David Williams issued a directive to hospitals in April to temporarily pause non-emergency procedures in order to ensure that the hospital system had enough capacity to cope with COVID-19 patients as hospitalizations mounted during the third wave.
Similar directives were issued during the first and second waves as well.
Officials said Wednesday that virtually all of the backlog from Wave 1 has been cleared, while around 80-90 per cent of the Wave 2 backlog has cleared. However those estimates do not account for people who were either not diagnosed or who did not seek treatment because of the pandemic.