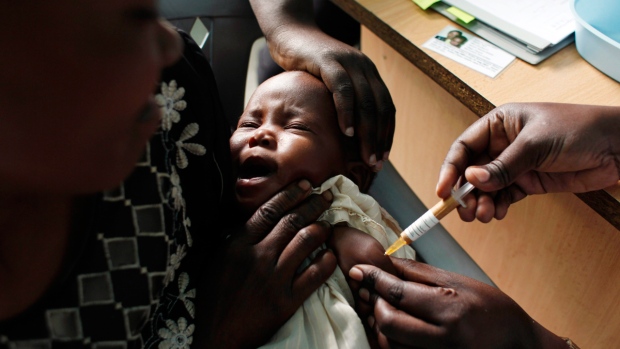
KAMPALA, Uganda - Health authorities in Kenya on Friday started administering doses of the world's only licensed malaria vaccine to young children in rural areas facing high transmission rates.
Kenya became the third African country to introduce the vaccine, after Malawi and Ghana. The aim is to reach about 360,000 children per year across the three countries.
The health ministry described the milestone on Twitter as “a historic day” for the East African country as the health minister launched vaccinations in remote Homa Bay county.
Malaria is a top killer in many African countries. According to the World Health Organization, the region accounted for 92% of the cases and 93% of malaria deaths in 2017. The parasitic disease kills about 435,000 people every year, most of them children under 5 in Africa.
The vaccine is the first and only vaccine to significantly reduce malaria in children, WHO said in a statement.
“Africa has witnessed a recent surge in the number of malaria cases and deaths. This threatens the gains in the fight against malaria made in the past two decades,” said Dr. Matshidiso Moeti, WHO regional director for Africa. “The ongoing pilots will provide the key information and data to inform a WHO policy on the broader use of the vaccine in sub-Saharan Africa. If introduced widely, the vaccine has the potential to save tens of thousands of lives.”
It took GlaxoSmithKline and partners more than 30 years to develop the vaccine, at a cost of around $1 billion. GSK is donating up to 10 million vaccine doses in the current vaccination initiatives.
Although the malaria vaccine only protects about one-third of children who are immunized, those who get the shots are likely to have less severe cases of malaria.
“I am sure the vaccine will help in reducing malaria and will cut the cost of going to the hospital every now and then,” said Newton Kawinio, a local traditional chief.
“By reducing the number of cases of malaria by 40% in the area where this has been rolled out, we are going to free up the number of resources in terms of health care workers in order to address other diseases, we are gonna save a tremendous number of lives,” said Dr. Aaron Samuels with the Centers for Disease Control and Prevention. “For every 200 children vaccinated, it's estimated that one child's life will be saved.”
Experts have begun testing out other new tools to fight malaria, including the development of genetically modified mosquitoes with an infertility gene.
Resistance is growing to medicines that treat the disease, while mosquitoes are becoming more resistant to insecticides. In addition, funding for malaria efforts has plateaued in recent years.
In neighbouring Uganda, health officials last month reported a surge in malaria cases as cases rise even among adolescents. They cited global warming and longer wet seasons for the increase.