The Ontario government is turning to other provinces and territories for nurses and health-care professionals to help “increasingly strained” hospitals that are grappling with a surge in COVID-19 patients.
In a letter obtained by CTV News Toronto, Ontario’s Deputy Health Minister Helen Angus wrote to all of her counterparts across the country about the strained hospital capacity in Ontario due to the deadly pandemic.
She said the province is “urgently” looking for health human resources and asked her counterparts if they could send mostly ICU nurses and other health-care professionals to Ontario to assist these overwhelmed hospitals.
The government estimates that Ontario might have a gap in staffing of around 4,145 nurses in the hospital sector alone over the next four months.
“I recognize the challenges all jurisdictions face as a result of the pandemic, but the challenges we are facing here in Ontario are such I feel I must seek to identify whether there are resources available in the country that could be directed to Ontario, if possible,” Angus wrote.
The government is seeking the assistance of 620 health-care professionals to support Ontario hospitals, including:
• 500 Nurses (ICU/Critical Care/recovery room/general)
• 100 Respiratory Therapists
• 10 Perfusionists (unregulated in Ontario)
• 10 Anesthesia Assistants (unregulated in Ontario)
Angus said the assistance is mostly needed in southern Ontario, particularly in COVID-19 hot spots in the Greater Toronto Area.
“We are projecting a need for this critical support for four months following the anticipated peak of the third wave; however, the length of the deployment is subject to COVID-19 case load and ICU capacity in the province,” she wrote.
Temporary relocation expenses will be provided to those deployed in Ontario.
Alberta responded to the letter later Friday morning saying it is "not in a position" to send their health-care workers out of the province.
"When the pandemic began, Alberta found itself in a surplus of PPE and shipped over 35 million units of gloves, masks, goggles, and ventilators to our friends in BC, Ontario, and Quebec. However, with COVID-19 cases and hospitalizations on a sharp rise here in Alberta, we are simply not in a position to send our health care workers outside the province at this time," Premier Jason Kenney's office said in a statement to CTV News.
"Our priority must be and will be the health and safety of Albertans, and that means making sure our hospitals are adequately staffed to treat COVID-19 patients."
Ontario's call for help comes as an intensive care physician in Toronto says ICU triage is “an eventuality,” as COVID-19 hospitalizations reach record highs.
Dr. Michael Warner, head of critical care at Michael Garron Hospital, has been very vocal recently about the need for the Ontario government to implement more restrictions to reduce hospitalizations as the health-care system is swamped with COVID-19 patients.
With a record 1,955 COVID-19 patients in Ontario hospitals in the past 24 hours and 701 of those in ICUs, Warner says hospitals are nearing the point of having to prioritize life-saving treatment based on a person's likelihood of surviving.
“I mean every hospital has gone through simulation of this. It's been socialized, it’s been practiced, it's our greatest fear, and I actually can't see a situation where some form of triage doesn't take place,” he told CTV News Toronto.
During the first wave of the pandemic last year, long-term care home residents and Ontarians over 80 years old were overwhelmingly infected and dying from the virus.
But with the highly-contagious variants of concern spreading across the province, Warner says younger patients are being admitted to hospitals and are at risk of not receiving critical care if triaging comes into effect.
“This is, you know, about 50 year olds not getting life support, not 80 year olds. Not that life is more important for one person than the other but the stakes are so much higher now, which is why we have to do everything to protect people from what I think is going to be an eventuality,” he said.
Ontario Health Executive Vice President Dr. Chris Simpson told CP24 earlier this week that the province’s health-care system could accommodate up to 900 COVID patients in intensive care through the halting of elective surgeries and the redirecting of some resources but may have to turn to the “last resort” of triage should the number rise above that.
Last week, hospitals outside of northern Ontario were instructed to begin “ramping down” elective surgeries and procedures as hospitals have been flooded with COVID-19 patients.
In January, hospitals received guidelines from the government on how to deal with critical care triage if there aren’t enough ICU beds. Under those guidelines, patients are ranked on their likelihood of surviving a year after the onset of critical illness. Those guidelines, however, have not been finalized.
On Friday, Chief Medical Officer of Health Dr. David Williams said if the number of patients hospitalized keeps rising then implementing triage protocol is possible.
"No one wants to put a triage system in place. But in other instances of pandemics where large epidemics hit populations, unfortunately there’s large percentages, of not only hospitalizations, but large percentages of deaths, more than we have seen in Ontario. We don’t want to go there. No one wants to go there but it is a reality," he said.
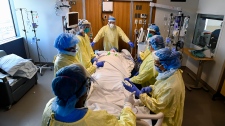
Warner’s grim statement comes as tents have been erected today at Toronto General Hospital and Toronto Western Hospital to provide more waiting space for patients.
“This reflects the increasing number of people with COVID symptoms and the tents are a response to the rise in people needing to be seen with appropriate distancing,” University Health Network said in a statement.
Yesterday, Premier Doug Ford’s cabinet met to discuss implementing additional measures, including a curfew and shutting down all construction projects that are not deemed critical infrastructure, sources told CP24 and CTV News Toronto.
Ford announced the extension of the stay-at-home order and additional restrictions Friday afternoon after the province’s COVID-19 science table releases new modelling data.
Warner said he has warned Ford about the severity of the situation in hospitals but that the government has failed to implement more measures fast enough to reduce spread of the virus.
“I texted him on March 26 saying that this is coming, and he needs to make changes, and that the modeling was clear on April 1, and here we are. And he had the modeling two days ago and the announcement’s at 2:30 [today]. Every second matters and I don't know why we're sitting on this.”
Warner argues that the government needs to act now to protect those who work in essential congregate settings, as they make up many of the sick patients infected with the virus.
“What we haven't done now, and we've avoided doing, and what has become a political issue where there's nothing political about it, is protect the people who are dying,” he said.
“And I'm not going to stop saying this until I stop intubating essential workers, take the politics out of it, just do the right thing and make sure everything that's non-essential is closed. Those who have to go to work need the best protection available, whether it's PPE, paid sick days, paid vaccination time, rapid testing in workplaces, it's not that complicated.”